Article Text
Abstract
Objective There were two primary objectives, namely: (1) to determine the social network types that Canadian adults aged 45 and older belong to and (2) to discover if social network type is associated with nutrition risk scores and the prevalence of high nutrition risk.
Design A retrospective cross-sectional study.
Setting Data from the Canadian Longitudinal Study on Aging (CLSA).
Participants 17 051 Canadians aged 45 years and older with data from baseline and first follow-up of the CLSA.
Results CLSA participants could be classified into one of seven different social network types that varied from restricted to diverse. We found a statistically significant association between social network type and nutrition risk scores and percentage of individuals at high nutrition risk at both time points. Individuals with restricted social networks had lower nutrition risk scores and are more likely to be at nutrition risk, whereas individuals with diverse social networks had higher nutrition risk scores and are less likely to be at nutrition risk.
Conclusions Social network type was associated with nutrition risk in this representative sample of Canadian middle-aged and older adults. Providing adults with opportunities to deepen and diversify their social networks may decrease the prevalence of nutrition risk. Individuals with more restricted networks should be proactively screened for nutrition risk.
- malnutrition
- nutritional status
- aging
- diet, food, and nutrition
- epidemiology
Data availability statement
Data may be obtained from a third party and are not publicly available. Data are available from the Canadian Longitudinal Study on Aging (www.clsa-elcv.ca) for researchers who meet the criteria for access to deidentified CLSA data.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
WHAT IS ALREADY KNOWN ON THIS TOPIC
Social factors such as social support and marital status have been associated with nutrition risk. However, most studies have looked at social factors in isolation. It is unknown how social network type affects nutrition risk.
WHAT THIS STUDY ADDS
Social network type is associated with nutrition risk, with individuals belonging to more restricted network types more likely to be at high risk.
HOW THIS STUDY MIGHT AFFECT RESEARCH, PRACTICE OR POLICY
Proactively screening individuals with restricted social networks may help prevent the progression from nutrition risk to malnutrition.
Introduction
Nutrition at midlife and beyond influences both health and optimal ageing.1 While there are many ways to define optimal ageing,2 it is commonly described as the maintenance of function across multiple domains (physiological, mental and social).3 Among the factors that can influence optimal ageing is nutrition risk, as low nutrition risk is associated with optimal ageing.4 5 Nutrition risk is the risk of poor nutrition status or nutritional depletion that occurs when food and/or nutrient intake do not meet needs.6 7 Numerous physiological, psychological and social changes or risk factors occur as people age that can result in nutrition risk.8 The consequences of increased nutrition risk include malnutrition, frailty, decreased quality of life, hospitalisation and higher mortality rates.6 9 10 In Canada, approximately one-third of adults aged 50 and older are at nutrition risk.11
Social relationships and social networks also influence optimal ageing.12 Social networks can be defined as ‘the web of social relationships that surround an individual and the characteristics of those ties’.13 Social networks have been shown to influence a number of health outcomes, both physical and psychological.13 Individuals belonging to more diverse network types tend to have better health outcomes, whereas individuals belonging to more restricted networks tend to have worse health outcomes.14–16
Social network characteristics (such as number of social network members, frequency of contact with network members, frequency of social participation) can be used to classify individuals into social network types that range from socially isolated to socially integrated.17 One Canadian study found that adults aged 65 and older belonged to one of six social network types: diverse, friend focused, family-friend, few children, few friends and restricted.17 They also found that social network type was associated with social support.17
Conceptual framework
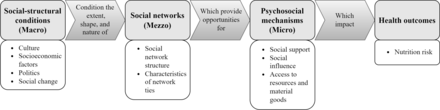
Our study uses social network theory, as described by Berkman et al, as its conceptual framework.13 This theory describes how social networks affect health outcomes, such as nutrition risk (figure 1). This framework posits that social and cultural contexts (macro level) influence social networks (mezzo level), which in turn affect social and interpersonal behaviour (microlevel). These psychosocial mechanisms (social and interpersonal behaviour) then impact health.13
Social network theory (adapted from Berkman et al13).
Characteristics of social networks include their size, range, density, boundedness, proximity, homogeneity and reachability. Characteristics of the ties within these networks include frequency of contact, frequency of participation, reciprocity of ties and duration of ties.13
Social networks affect health outcomes, such as nutrition risk, through psychosocial mechanisms, which include social support, social influence and access to resources and material goods.13 Social networks may influence nutrition risk through several of these psychosocial mechanisms. Eating with others improves dietary intake and reduces nutrition risk.18 Individuals with larger social networks and greater levels of social participation may have more opportunities to eat with others and to have social norms around food reinforced.18 Some studies have found that social support helps reduce nutrition risk, likely because individuals with increased social support have greater assistance with food-related activities, such as meal preparation and grocery shopping.18 Access to resources, in the form of income, has been associated with nutrition risk,19 as individuals with higher incomes have an easier time affording adequate amounts of healthy food.20 However, a few studies have examined the relationship between social network types and nutrition. One study from the UK found that social network type was associated with nutritional status, measured using the Mini Nutritional Assessment-Short Form (MNA-SF).21 Participants who were in, or moving to, more restricted network types had low MNA-SF scores, and thus poor nutritional status.21 A study of frail older adults in South Korea found that social network type was associated with diet quality.22 Participants belonging to more restricted networks had lower diet quality compared with those with larger social networks.22
Currently, it is unknown how social network type affects nutrition risk in Canadian adults at midlife and beyond. If social network types affect nutrition risk, this information can inform programmes and policies designed to reduce the prevalence of nutrition risk and improve nutritional status. It can also help to identify individuals who should be screened proactively for nutrition risk. As nutrition risk occurs before malnutrition, and because it is easier to treat nutrition risk compared with malnutrition, it is important to identify those who should be screened for nutrition risk.23 24
There were two primary objectives of this research, namely: (1) to determine the social network types that Canadian adults aged 45 and older belong to, using the factors at the mezzo level of Berkman et al’s social network theory13 and (2) to discover if social network type is associated with nutrition risk scores and the prevalence of high nutrition risk.
Materials and methods
Data source
The Canadian Longitudinal Study on Aging (CLSA) is a large, Canadian longitudinal study of more than 50 000 individuals who were between the ages of 45 and 85 when recruited.25 Recruitment and baseline data collection were completed in 2015, and the collection of first follow-up data were completed in 2018. Participants will be followed every 3 years for 20 years or until participant death.25
Briefly, there are two cohorts of participants, tracking and comprehensive. There are 21 241 tracking participants followed by telephone interview only, and 30 097 comprehensive participants who are interviewed in person, undergo physical assessments and provide urine and blood samples.25 Participants in the tracking cohort were randomly selected within age and sex strata in each province. The proportion of individuals in the tracking cohort from each province is proportional to the province’s population to allow the data gathered to be generalised to the Canadian population and a given province’s population.25 For this reason, our study uses data from the tracking cohort.
The selection and recruitment process for the CLSA has been described elsewhere.25 In brief, for CLSA tracking participants, three sampling frames were used: a subset of participants from Statistics Canada’s Canadian Community Health Survey-Healthy Aging (CCHS-HA), registries of provincial healthcare systems and random digit dialling of landline telephones.26 As individuals with lower socioeconomic status and less education are often under-represented in population-based studies, there was an attempt to oversample certain regions identified from census data to ensure representation of these groups.26
The full list of CLSA measures has been reported elsewhere.25 Briefly, there is a core set of questionnaires that are common across both cohorts. These measures cover many domains including sociodemographics, social, physical, health status, psychological and health service use.26 We mapped data from the CLSA to Berkman et al’s social network theory13 (table 1). We used baseline data for all the variables, except for nutrition risk, where we used data from both baseline and first follow-up. The measures that we used in our study are described below.
Mapping CLSA variables onto Berkman et al’s social network theory
Demographics
Demographic measures included age, sex assigned at birth, marital status, education and income. The demographic measures were adapted from those administered in the CCHS-HA study. Sex assigned at birth had male or female as the options. Participants reported their marital status according to the following categories: married/common-law, single (never married), divorced, separated or widowed. We combined these into three categories: married/common law, single (including single, divorced or separated) and widowed. Participants were asked about their highest level of education; this was categorised as less than secondary school graduation, secondary school graduation, some postsecondary and postsecondary degree/diploma. Participants reported their household income from all sources using the following categories: less than CDN$20 000, CDN$20 000–CDN$49 999, CDN$50 000–CDN$99 999, CDN$100 000 or more.
Social network size
Participants were asked to indicate the number of people in each of these groups: children (biological, adopted, step), siblings, close friends, relatives and neighbours. Participants were also asked to indicate the number of people known through work or school, the number of people known through community involvement and the number of people known through other activities. For each of these variables, we placed participants into quartiles.
Frequency of contact with network members
Participants were asked when they last got together with children, siblings, close friends, relatives and neighbours. The options were: more than 1 year ago, within the past year, within the past 6 months, within the past month, within the last week or 2, within the last day or 2 and live with me; the last two were combined into a single category.
Social participation
Social participation was measured using items used in the CCHS-HA and the English Longitudinal Study of Ageing. These items have undergone rigorous development and testing.27 28 Participants were asked how often they participated in eight different types of activities over the past 12 months. These activities were: family/friend activities, religious activities, sports or physical activities with others, education or cultural activities, clubs or fraternal organisations, association activities, volunteer or charity work and other recreational activities. Options were never, at least once a year, at least once a month, at least once a week and at least once a day, with a numeric value of 0 (never) to 4 (at least once a day) assigned during analysis. We summed the responses from each of the categories to create a social participation variable that could range from 0 to 32, with higher numbers indicating greater frequency of participation. We then divided this variable into quartiles.
Nutrition risk
Nutrition risk was measured using the abbreviated version of Seniors in the Community: Risk Evaluation for Eating and Nutrition (SCREEN) II (rebranded as SCREEN-8).29 It includes eight questions ask about eating habits on a typical day. There are questions about weight change, skipping meals, appetite, swallowing, servings of fruit and vegetables, fluid intake, eating with others and meal preparation.29 SCREEN-8 scores can range from 0 to 48.30 When compared with registered dietitians’ assessment of nutritional risk, SCREEN-8 has good specificity and sensitivity (Area under the curve ≥78%). SCREEN-8 has strong test–retest reliability within 2 weeks with Intraclass correlation coefficient (ICC)=0.84, and the inter-rater reliability is also strong with ICC=0.79.30 A SCREEN-8 score less than 38 indicates that an individual is at high nutrition risk,30 thus higher scores indicate lower nutrition risk and lower scores indicate higher nutrition risk.
Data analysis
We started by examining the descriptive statistics for each of the variables used in our analysis. We reported means and SDs for continuous variables and percentages for categorical variables. We examined the percentage of missing data and used Little’s Missing Completely at Random (MCAR) test31 to determine if data were MCAR.
Deriving social network type
Using a person-centred approach, we derived social network types using latent class analysis (LCA). LCA is used to determine if different unobserved subgroups, known as latent classes, exist within a population.32 33 The latent classes are derived using a set of categorical or ordinal variables that are observed and available in a dataset.32 33
Using social network theory as described by Berkman et al,13 we considered the following variables for the LCA: social network structure (number of close friends, siblings, relatives, children, neighbours, number of people known through work or school, number of people known through community involvement, number of people known through other activities), characteristics of network ties (frequency of contact with close friends, siblings, relatives, children, neighbours) and social participation (frequency of participation in community activities).
We used RStudio34 and the package poLCA35 to derive the latent classes. We estimated a series of models ranging from four to eight classes as previous research has found between four and eight social network types.15 17 36 37 We noted the evaluation metrics for each model, including Bayesian Information Criterion (BIC), sample-size adjusted BIC (SABIC), consistent Akaike information criterion (cAIC) and entropy.32 Lower values for BIC, SABIC and cAIC indicate better fit.32 Entropy values closer to one are best.32
We calculated the mean and SD for each of the variables used in the LCA for each of the solutions from two to eight classes. For each class, we noted means that were 0.5 and 0.25 SDs above and below the mean for each variable. Since classes need to make conceptual sense to be useful,17 we examined each solution to determine which number of classes made sense in terms of the variables used to derive the classes. We used this information, combined with the evaluation metrics from the LCA solutions, to determine the appropriate number of classes.
To understand and label the different classes, which represent different social network types, we examined the variables that differed the most between classes. Similar to previous research looking at different social network types,17 36 we indicated which variables in each cluster are 0.5 SD (bold) or 0.25 SDs (italics) above or below the mean.
Next, we examined whether the classes varied on demographic measures, social support and health-indicator variables. We used χ2 tests to determine whether the classes differed on sex, marital status, household income, and educational attainment, and one-way analysis of variance (ANOVA) to determine whether the clusters differed on age. To examine the effect size, we used Cramér’s V for categorical variables and η2 for continuous variables.38 For all ANOVA tests, if Levene’s test indicated that the assumption of homogeneity of variances was violated (p<0.001), we used Welch’s ANOVA.
Social network type and nutrition risk
We examined whether nutrition risk scores, as measured using SCREEN-8, at both baseline and first follow-up differed by classes (social network type). We conducted an ANOVA test for the SCREEN-8 scores at baseline and follow-up, using the social network types created as the grouping variable. We used η2 to examine the effect size. Next, we conducted a χ2 test to determine whether the classes differed by percentage of individuals at high nutrition risk, using a SCREEN-8 cut-off score of 38.29 30
We ran two multivariable linear models, one with SCREEN-8 score at baseline and one with SCREEN-8 score at follow-up as the dependent variables. The social network types were the independent variables, and we controlled for demographics. Then two binomial logistic regression models were run, one with the presence of high nutrition risk at baseline and one with the presence of high nutrition risk at follow-up as the dependent variables. Once again, the social network types were the independent variables and we controlled for demographics.
Results
Sample description
In total there were 17 051 participants. The mean age of participants was 62.5 years (SD=10.4, range=44–88) and 52.2% were female (additional demographic details are found in tables 2 and 3). The mean baseline SCREEN-8 score was 39.04 (SD=6.17) and the mean SCREEN-8 score at follow-up was 38.00 (SD=6.57). At baseline, 33.9% of the sample was at high nutrition risk, and 41.1% were at high nutrition risk at follow-up. Between baseline and first follow-up, 17.6% of participants who were not at high nutrition risk at baseline developed high nutrition risk and 22.9% who were at high risk at baseline remained at high nutrition risk.
Social network types in the CLSA at baseline with means and SDs reported for each social network variable
Demographic variables for the different social network types
When we examined the proportion of missing data in our dataset, we were missing SCREEN-8 scores for 13.1% of the sample at baseline and 19.7% at follow-up (online supplemental table 1). Little’s MCAR test was not statistically significant (χ2=29 703.91, p=0.39), therefore we report the complete case analysis here.
Supplemental material
Latent class analysis
When we examined the evaluation metrics (table 4), the eight class solution appeared to be the best solution, but only slightly better than the six or seven class solutions, and all three had acceptable entropy. When we examined the means and SDs for the analysis variables for each of the six, seven and eight group solutions, the seven-cluster solution made the most conceptual sense given our mapping of CLSA variables onto Berkman et al’s social network theory.
Latent class analysis evaluation metrics
We show the means and SDs for all the variables used to determine the seven groups (table 2). We show unstandardised values to aid in interpretation. The seven social network types we derived are labelled diverse, friend focused, few friends, family focused, community focused, close family and restricted. These descriptors were based on the unique profiles of each cluster.
The seven social network types differed significantly from each other for all the demographic variables (table 3), as all ANOVAs and χ2 were significant at p<0.001, however, the effect sizes were small. In brief, the seven social network types can be characterised as follows:
Friend focused (21.5%)—few siblings, few relatives, low frequency of contact with siblings, high participation in community activities
Few friends (18.6%)—few friends and neighbours, low social participation, few people known through community involvement or other activities
Diverse (14.1%)—many network members, high frequency of contact with members, high participation in community activities, high proportion married, high levels of social support, low proportion live alone.
Family focused (13.7%)—youngest age group, many siblings and relatives, high frequency of contact with children, siblings and relatives.
Community focused (13.4%)—few siblings, many close friends, many people known through work or school, through community involvement, or through other activities, high participation in community activities.
Close family (11.4%)—many children, siblings and relatives, low frequency of contact with relatives.
Restricted (7.2%)—the oldest group, with few network members, low frequency of contact with network members, low participation in community activities, high proportion live alone, lower educational attainment, lower income, low levels of social support.
Social network type and nutrition risk
Social network type and nutrition risk at baseline
When we ran the ANOVA to determine if SCREEN-8 scores at baseline varied according to social network type, Levene’s test indicated that the assumption of homogeneity of variances was violated (p<0.01). We, therefore, used Welch’s ANOVA. SCREEN-8 scores were significantly different for different social network types, (Welch’s F(6, 6186.31) = 60.08, p<0.001) (table 5). The effect size was small (η2=0.025, 95% CI 0.020 to 0.029).38 The diverse group had the highest SCREEN-8 scores (40.19, SD=5.53), indicating that they were the least likely to be at high nutrition risk. The restricted group had the lowest SCREEN-8 scores (37.07, SD=7.44).
Nutrition risk for different social network types
The results of the χ2 test of independence between social network type and high nutrition risk at baseline indicated that there was a statistically significant association between social network type and high nutrition risk, although the effect size was small (χ2(6) = 207.11, p<0.0001, Cramér’s V=0.113, p<0.001). The diverse group had the lowest percentage of individuals at nutrition risk (27.2%), and the restricted and few friends groups had the highest percentage of individuals at nutrition risk (42.5%).
Social network type and nutrition risk at follow-up
The ANOVA examining whether SCREEN-8 scores at follow-up varied according to social network type was statistically significant (Welch’s F(6, 6535.20) = 64.94, p<0.001). The effect size was small (η2=0.024, 95% CI 0.020 to 0.029).38 At follow-up the diverse group had the highest SCREEN-8 scores (mean=39.52, SD=5.90) and the restricted group had the lowest SCREEN-8 scores (mean=35.88, SD=7.54).
The results of the χ2 test of independence between social network type and nutrition risk at follow-up indicated that there was a statistically significant association between social network type and nutrition risk, although the effect size was small (χ2(6) = 237.92, p<0.0001, Cramér’s V=0.118, p<0.001). As at baseline, the diverse group had the lowest percentage of individuals at nutrition risk (30.2%) The restricted group had the highest percentage of individuals at nutrition risk (52.0%).
Social network type and nutrition risk, controlling for demographics
The regression model predicting SCREEN-8 scores at baseline, using social network type and controlling for demographics, was statistically significant (F (16, 13384) = 60.65), R2=0.068, p<0.001. Among the social network types, the diverse, family focused, community focused, close family-focused and friend-focused groups, compared with the restricted group, were statistically significant predictors of SCREEN-8 scores at baseline (online supplemental table 2). The regression model predicting SCREEN-8 scores at follow-up, using social network type and controlling for demographics, was statistically significant (F (16, 13930) = 58.52), R2=0.063, p<0.001. Among the social network types, the diverse, family focused, community focused, close family-focused and friend-focused groups, compared with the restricted group, were statistically significant predictors of SCREEN-8 scores at follow-up (online supplemental table 3).
The binomial logistic regression model predicting the presence of high nutrition risk at baseline was statistically significant (χ2(16) = 803.01, p<0.001, Nagelkerke R2=0.70). Compared with the restricted group, the diverse group had 0.64 lower odds of being at high nutrition risk at baseline, and the close family group had 0.71 lower odds of being at high nutrition risk at baseline (online supplemental table 4). The binomial logistic regression model predicting the presence of high nutrition risk at follow-up was statistically significant (χ2(16) = 831.87, p<0.001, Nagelkerke R2=0.67). Compared with the restricted group, the diverse group had 0.67 lower odds of being at high nutrition risk at follow-up (online supplemental table 5).
Discussion
To our knowledge, this is the first study to examine social network types and nutrition risk in Canada and more specifically using data from the CLSA. Our findings provide an important contribution to the understanding of social networks and nutrition risk. After deriving social network types that classified Canadian adults aged 45 years and older into one of seven social network types, we found that social network type was associated with nutrition risk scores as measured by SCREEN-8 at both baseline and follow-up and that social network type was associated with the presence of high nutrition risk at both baseline and follow-up. This study lends further support for Berkman et al’s social network theory13 that posits social networks provide social support, social influence, social engagement and access to resources, which in turn affect health behavioural pathways, such as diet, which will then have an impact on nutrition risk.
We found that the diverse group had the highest SCREEN-8 scores at baseline and follow-up. The restricted group had the lowest SCREEN-8 scores at both time points. Similarly, the diverse group had the lowest percentage of individuals at high nutrition risk at baseline and at follow-up. The restricted group had the highest percentage of individuals at risk at both time points. The community focused group had the second highest SCREEN-8 scores at both time points, and the second-lowest prevalence of high nutrition risk at both time points. This group had few family members, but many friends, high participation in community activities and many people known through work or school, community involvement and other activities. Thus, relationships beyond family are important when it comes to preventing the development of high nutrition risk.
Previous research has found that infrequent social participation was associated with high nutrition risk in adults aged 65 and older.19 Other studies have found that those with close relationships are less likely to be at nutrition risk.39–42 Close relationships may provide greater opportunities to share meals or to share resources for food-related activities such as grocery shopping and meal preparation. Eating with others has been shown to improve dietary intake and reduce nutrition risk.18 43 Receiving assistance with food-related activities, if such assistance is required, can also help reduce nutrition risk.18 44 The larger an individual’s social network and the greater frequency of contact with others within that network, the greater the opportunities to eat with others or to receive assistance with food-related activities. This could be why individuals in the diverse network have the lowest nutrition risk and individuals in the restricted network have the highest nutrition risk.
Similar to previous research,17 36 45 46 we found that social networks ranged from diverse (large size, broad range, high frequency of contact, high frequency of participation) to restricted (small size, limited range, low frequency of contact, limited participation). Unlike Harasemiw et al,17 we found seven different social network types rather than six. There are likely three reasons for this difference. First, our sample included adults aged 45 and older, whereas Harasemiw et al only examined adults aged 65 and older. Social network type has been associated with age in previous research.16 Second, we included additional variables in our analysis (the number of relatives and the frequency of contact with relatives, number of people known through work or school, community involvement and other activities), which they did not. We included these variables as they were elements in Berkman et al social network theory.13 Third, we used LCA to derive our social network types, whereas they used k-means cluster analysis.
We purposely included middle-aged adults so that in the future we can examine how social networks change as people enter older adulthood, as CLSA participants are followed every 3 years for 20 years or until participant death.25 Those in younger age groups may also be more likely to be living with partners and may still have children living at home. Thus, they may have closer ties with family members living at home.
In addition to the diverse group and the restricted group, we also found a friend-focused group and a family-focused group; both have been found in previous studies.14 36 We also found a close family group, similar to Cohn-Schwartz et al,47 and similar to Harasemiw et al,17 we found a few friends group. Thus, these social network types appear to be present in some populations, but not necessarily in all populations.
In contrast with other studies, we also found a community-focused group. This could be due to the fact that different clustering methods may produce different results.48 Different data sets and inclusion of different variables in the clustering procedure will also produce different results. We included variables that reflected connections in the wider community: number of people known through work and school, through community involvement and through other activities. Nevertheless, the fact that numerous studies report both diverse, restricted and friend-focused groups,14–16 36 45 49 50 indicates that these three social network types are likely stable across different populations and different age groups.
A strength of this study is the use of CLSA data, which provides a nationally representative sample of community-dwelling Canadians aged 45–85.26 The CLSA asked questions about the size, range and density of participants’ social networks and their participation in community activities, enabling us to derive the social network types or groups that individuals belonged to. Additionally, the CLSA measured nutrition risk with a valid and reliable tool for determining nutrition risk in community-dwelling adults that matches well with registered dietitian determination of nutrition risk.30
One weakness of our study is the lack of measures for contact with network members other than in-person gatherings. While the CLSA did ask about frequency of using social networking sites to stay in touch or make plans with friends and with family, for these questions there was a large amount of missing data, so we excluded those questions from our analysis. The CLSA also did not include any questions about frequency of contact using other means, such as email, telephone, video chats or other virtual means of communication. Another limitation of our study is that we only adjusted for demographic variables in our regression analyses. Future research should include other potential confounders such as physical health, alcohol use and smoking behaviour. Future research should examine social network type and nutrition risk while controlling for additional covariates.
It should be noted that we cannot imply causation, however this study does demonstrate that social network type is associated with SCREEN-8 scores and the presence of high nutrition risk at two time points, 3 years apart. Social network type at baseline was found to predict nutrition risk at first follow-up. Due to the cross-sectional nature of the data, we cannot state that social network type causes the differences in nutrition risk observed between the different network types. It is possible that nutrition risk influences social network type or that they are both influenced by other factors. As the CLSA is a longitudinal study, future research will be able to examine how social network types and nutrition risk influence each other over time.
Another consideration is our use of LCA to derive the social network types. It is possible a different method could have come up with different solutions. Similarly, other researchers looking at the same classes could have given the social network types different labels based on their interpretations of the results.
Conclusion
We found that community-dwelling Canadians aged 45 and older belong to a wide variety of social network types, ranging from diverse to restricted. We found that social network type is associated with SCREEN-8 scores and the prevalence of high nutrition risk, with individuals who have more diverse social network groups having lower nutrition risk and individuals who have more restricted social network groups having increased nutrition risk. Providing individuals with opportunities to expand and deepen their social networks (eg, by making it easy to engage in community activities that provide opportunities to meet with others) may therefore help to improve nutrition risk in community-dwelling middle-aged and older adults. Additionally, individuals who work with middle-aged and older adults should be aware that individuals with more restricted social networks may be at higher risk for poor nutrition status, and proactively screen them for nutrition risk. Further research should examine how social network types change with age, and how social network types affect changes in nutrition risk over time. It should also explore how social networks influence nutrition risk as middle-aged adults transition into older adulthood.
Data availability statement
Data may be obtained from a third party and are not publicly available. Data are available from the Canadian Longitudinal Study on Aging (www.clsa-elcv.ca) for researchers who meet the criteria for access to deidentified CLSA data.
Ethics statements
Patient consent for publication
Ethics approval
Ethics approval was granted by Queen’s University Health Sciences and Affiliated Teaching Hospitals Research Ethics Board REH-722-18. Participants gave informed consent to participate in the study before taking part.
Acknowledgments
This research was made possible using the data/biospecimens collected by the Canadian Longitudinal Study on Aging (CLSA). Funding for the Canadian Longitudinal Study on Aging (CLSA) is provided by the Government of Canada through the Canadian Institutes of Health Research (CIHR) under grant reference: LSA 94473 and the Canada Foundation for Innovation, as well as the following provinces, Newfoundland, Nova Scotia, Quebec, Ontario, Manitoba, Alberta, and British Columbia. This research has been conducted using the CLSA Baseline Tracking Dataset—V.3.7, and Follow-up 1 Tracking Dataset—V.2.2, under Application Number 2104008. The CLSA is led by Drs. Parminder Raina, Christina Wolfson and Susan Kirkland. The AB SCREENTM II, rebranded as SCREEN-8, assessment tool is owned by Dr. Heather Keller. Use of the AB SCREENTM II assessment tool was made under license from the University of Guelph.
References
Supplementary materials
Supplementary Data
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
Footnotes
Twitter @ChrisMillsRD
Contributors CMM is the guarantor of this work, and planned the study, performed all statistical analyses, completed the data analysis, and wrote the paper. CD helped to plan the study, supervised the data analysis, and helped revise the manuscript. HHK and VGD helped to plan the study and revise the manuscript.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests CMM is supported by scholarships from Queen’s University and Support Our Troops. HK is past chair/co-chair of the Canadian Malnutrition Task Force (CMTF), currently leads the Primary Care working group at CMTF, and is the creator of the SCREEN-8 tool used in this research. CD and VGD declare no conflicts of interest.
Provenance and peer review Not commissioned; externally peer reviewed.
Supplemental material This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.